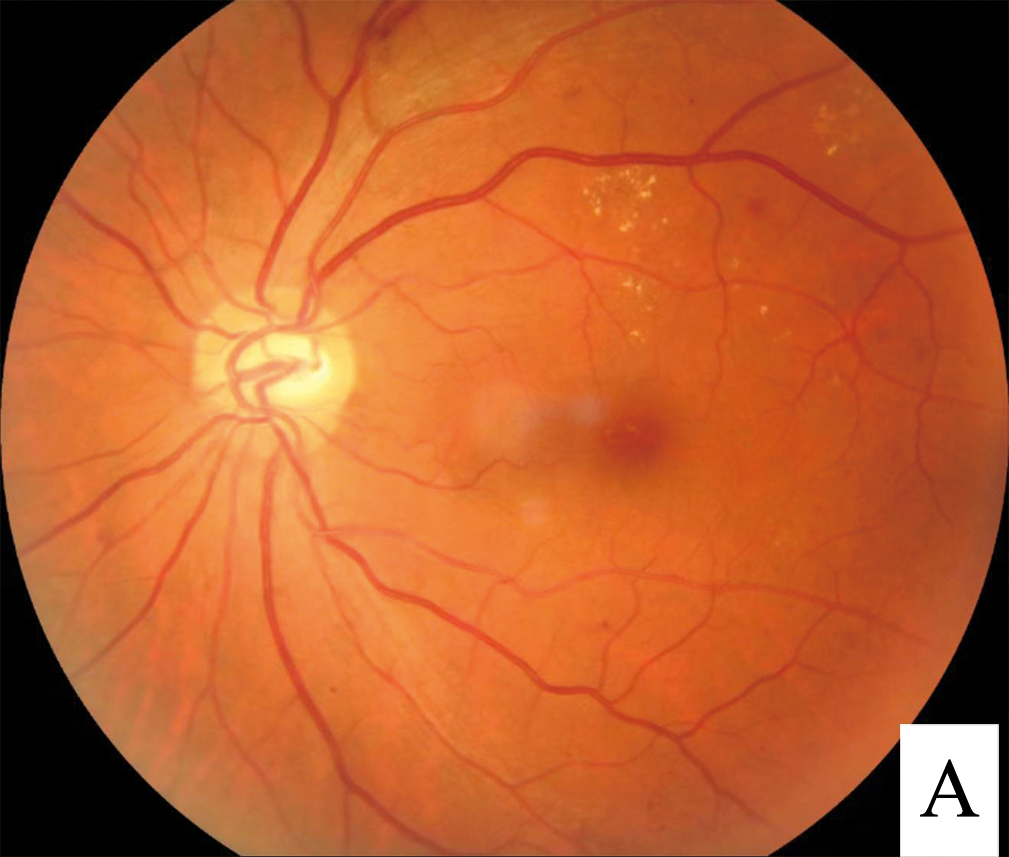
A Complete Guide to Diabetic Macular Edema
The abnormal leakage of blood or body fluids into the macula from retinal blood vessels that are damaged and leaky causes diabetic macular edema. Blood vessels damaged by high blood sugar levels seep into the macular. The diagnostic procedures for this disease include:
- The visual acuity test.
Dilated eye exam.
Fluorescein angiography.
Optical coherence tomography.
The Amsler grid test.
Treatment for Diabetic Macular Edema (DME)
Pharmaceuticals are the first line of treatment for DME. The type of disease, such as centrally involved DME or non-centrally involved DME, determines the course of treatment.
Anti VEGF Injections
An anti-vascular endothelial growth factor (anti-VEGF) drug is frequently used as the first-line treatment for centrally involved diabetic macular edema (CI-DMO). The most common cause of vision loss in people in their working years is diabetic macular edema (DME), primarily caused by vascular endothelial growth factor (VEGF). Although most eyes can benefit from anti-VEGF efficacy, a significant portion does not respond well enough, and many continue to receive this therapy long after it can be effective. An ophthalmologist performs the treatment by administering the injection directly into the vitreous cavity in the back of your eye.
Use of Corticosteroids
Worldwide, diabetic macular edema (DME) continues to be a significant factor in vision loss. Some patients with advanced or recurring DME may benefit from corticosteroids, regarded as second-line therapy for DME. All steroids carry the risk of cataract development and increased intraocular pressure. Additionally, intravitreal injection of any medicine takes hazards, including infected endophthalmitis. Of note is that the United States Food and Drug Administration has not yet approved any steroids for treating DME.
Laser Treatment
Macular laser therapy (MLT) was the cornerstone of diabetic macular edema treatment for over three decades before anti-VEGF therapy. DME has been classified as either focal or diffuse morphologically, but both can occasionally coexist in the eyes. Diffuse DME appears more resistant to focal and grid laser photocoagulation, whereas focal DME responds better to focused laser photocoagulation. The closure of leaky microaneurysms, retinal pigmented epithelium stimulation, initiating endothelial division, lowering oxygen consumption, and enhancing choroidal oxygen diffusion are some potential processes by which macular laser therapy improves diabetic macular edema.
Vitrectomy Surgery
It must be acknowledged that there is still much to learn about vitrectomy’s impact on DME. Beyond the mechanical removal of the vitreous, we are only now starting to comprehend the physiological ramifications of vitrectomy in DME. It can be helpful to determine whether the pathology is brought on by traction, the edema itself, ischemia, fluorescein angiography, and high-resolution optical coherence tomography.
This knowledge can assist us in identifying the primary cause or sources of the harm. When an eye has experienced extensive bleeding that has not healed, many patients find that a vitrectomy improves their eyesight. Vitrectomy carries a risk of developing an eye cataract in adults over 50.
As a systemic disease, diabetes mellitus can cause both macrovascular and microvascular problems. The management of patients with diabetes mellitus necessitates a comprehensive strategy that includes screening for diabetes complications, diabetes education, a focus on lifestyle modification, reasonable glycemic control, reducing cardiovascular risk, and avoiding drugs that can exacerbate lipid or glucose metabolism.
The progression of complications can be slowed down, and the quality of life can be increased with complete diabetes control. Learning about diabetes is crucial to managing the condition, but educating the patient about this chronic illness is even more critical. Knowledge and understanding are part of the treatment for better management of this disease.